Proper Nutrition For Inflammatory Bowel Disease
The key to proper nutrition for inflammatory bowel disease is to adapt to the symptoms and stages of the individual patient.

Malnutrition is common in people who have digestive problems. However, in inflammatory bowel disease, proper nutrition is key to reducing and relieving symptoms. We’ll tell you everything you need to know about it.
What are Inflammatory Bowel Diseases?
The digestive tract can suffer from various ailments that affect the state of health. For example, one of them is inflammatory bowel disease (IBD). This is a term for chronic diseases of the digestive tract of unknown cause, which then lead to inflammation.
The two most common IBDs are chronic ulcerative colitis (CUC) and Crohn’s disease (CD). There is also a third condition known as indeterminate colitis. This shares features of the previous two and can occasionally be identified as one or the other of the two as it progresses.
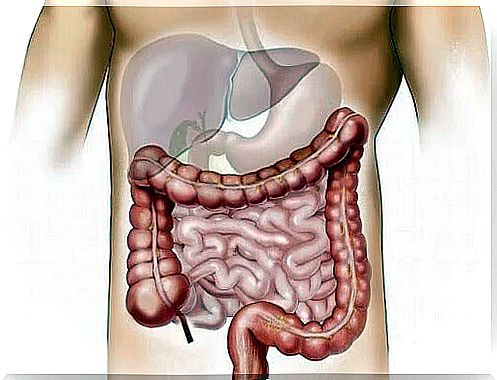
What are typical characteristics of inflammatory bowel disease?
Crohn’s disease
In this case, any part of the gastrointestinal tract can be affected, but the most common areas are the distal small intestine and the ascending colon. Injuries occur in certain areas and can damage all layers of the intestinal wall.
Ulcerative colitis
This disease only affects the colon and rectum. The injuries occur continuously and affect the mucous membrane and the connective tissue layer. This changes the function of the immune system of the digestive tract and thus causes a persistent inflammatory reaction.
What are the symptoms?
The most common symptoms of both diseases are severe colic and chronic bloody diarrhea. This then leads to weight loss, malnutrition, fever and skin and joint injuries.
Injuries to the intestinal lining cause several related nutritional problems, such as:
- anorexia
- Edema
- anemia
- Dehydration
- Loss of proteins and vitamins
- Change and imbalance in the mineral balance (zinc, iron, magnesium, calcium and selenium)
Causes of Malnutrition
Malnutrition is caused by several factors, such as:
- Decreased food intake
- The disease itself, which causes pain, diarrhea and vomiting
- Exclusion of certain foods
- Increased need due to fever, stress and loss of protein
- Malabsorption of nutrients
- Interaction between drugs and nutrients. According to the Spanish Foundation for the Digestive System, anti-inflammatory drugs, corticosteroids, immunosuppressants and antibiotics are used to treat these conditions.
What should the right diet look like for inflammatory bowel disease?
It must be remembered that IBD has phases when symptoms are weaker and phases when acute symptoms are more common. Therefore, the diet should always be tailored to the phase of life in which we are currently. Unless symptoms are present, the healthy eating plan does not need to include unnecessary restrictions.
In acute phases, the diet should be adapted to the nutritional requirements. It is important to eat several meals throughout the day, drink enough water and avoid extreme cold.
Diets low in short chain carbohydrates or FODMAP are beneficial in treatment. The diet should then contain the following proportions:
- 50% to 60% calories in carbohydrates
- 15 to 20% protein
- 25 to 30% fats (limit in case of diarrhea)
We must not forget that in some cases severe malnutrition with compromised bowel can develop. Then there is the option of parenteral or central nutrition.

Foods to avoid in acute symptoms
When we are in a phase of acute symptoms, avoid all foods that could cause gas and discomfort. These are for example:
- Legumes and cereals
- Dairy products, mainly milk
- Potatoes, sweet potatoes, corn, cassava, garlic, onions, cabbage
- Hard and spicy cheeses
- Fresh and dried fruits
- Honey, sugar, candies, syrups and jams that are sweetened with certain sweeteners such as xylitol or sorbitol
- Processed meat and sausage products and derivatives
- Alcoholic beverages, sodas, fermented beverages and coffee
- spicy or spicy dishes
In addition, it should be checked whether there is a vitamin or mineral deficiency. In these cases, dietary supplements can be beneficial.
Proper nutrition for inflammatory bowel disease when there are no acute symptoms
For all of the above, if the symptoms go away, it is important to gradually reintroduce the restricted foods. Then generally start with the following:
- Cooked vegetables that contain soluble fiber, such as: pumpkin, carrots, beetroot, zucchini
- Steamed or baked fruits, such as: apple, ripe banana, apricot, peach, pear
- Refined grains and derivatives
- Low-fat meats such as fish and chicken
One must consider that the progress through the change in diet can take several weeks and depends on the individual patient. The length of time between one and the other phase depends on the patient’s symptoms. In summary, the key to proper inflammatory bowel disease nutrition is to adapt it to the patient’s symptoms and stages.